Sleep is Medicine
The Double Whammy
- ADHD: Circadian Rhythm Delay. Their brain doesn’t make melatonin until 2 AM.
- Bipolar: Sleep disruption is the #1 trigger for mania.
- Result: A teen who can’t fall asleep, and whose lack of sleep triggers a manic episode where they don’t need sleep.
The Broken Clock: Circadian Rhythm in AuDHD + Bipolar
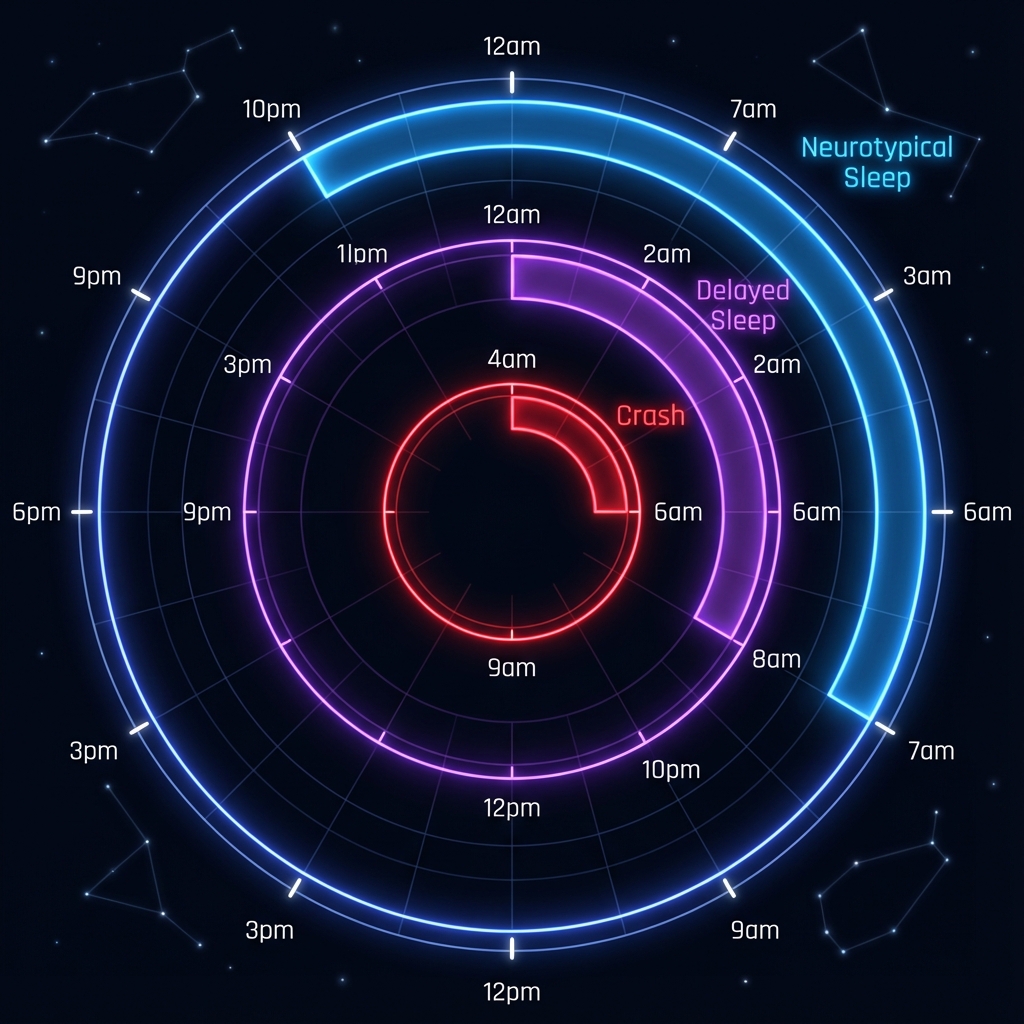
Notice how the AuDHD+Bipolar teen’s sleep window shrinks to 2 hours during mania. This is not “just” ADHD—this is a medical emergency.
Case Study: Alex’s All-Nighter
Alex Miller (14) is coding. It’s 3 AM. “Alex, go to bed,” his mom says. “I can’t. I’m in the flow. I’ll sleep later.”
By Thursday, Alex hasn’t slept in 56 hours. He’s giggly, then irritable, then convinced he’s “solving climate change with Python.”
His mom, Sarah, calls the psychiatrist. “Is this mania?”
“How long has he been awake?”
“Three days.”
“Yes. This is mania. Bring him in.”
The Science: Why Sleep Matters More for Bipolar Brains
Normal Sleep Cycle
- Melatonin rises → Brain signals “time for bed”
- Body temperature drops → You get sleepy
- Deep sleep → Brain clears waste, consolidates memory
- REM sleep → Emotional regulation processing
Bipolar + ADHD Sleep Disruption
- Melatonin doesn’t rise (ADHD circadian delay)
- Brain stays activated (racing thoughts from mania)
- No deep sleep → Emotional dysregulation worsens
- No REM → Mood destabilizes further
Result: A vicious downward spiral. No sleep → mania → less sleep → worse mania.
Protocol: The Dark Therapy Schedule
Dark Therapy = Controlled light exposure to force circadian rhythm reset. Research shows that blocking blue light in the evening can stop mania in its tracks. A randomized controlled trial found that patients using blue-blocking glasses saw a significant reduction in manic symptoms within just 3 days compared to placebo (Henriksen et al. 2016).
- The Mechanism: Blue light suppresses melatonin. By blocking it, we trick the brain into thinking it’s night.
The Why
Blue light (from screens, overhead lights) suppresses melatonin. For teens with ADHD, this delay is WORSE. For teens with bipolar, it can trigger mania.
Solution: Eliminate blue light 3 hours before target sleep time.
Hour-by-Hour Schedule (For 10 PM Bedtime)
7:00 PM: BEGIN DARK THERAPY
-
- Brands: Swanwick, TrueDark, Uvex (cheap on Amazon)
- Teen wears these until bedtime
8:00 PM: WIND-DOWN ACTIVITIES
9:00 PM: MELATONIN DOSE
9:30 PM: SLEEP HYGIENE
10:00 PM: LIGHTS OUT
10:30 PM: IF STILL AWAKE
Melatonin Dosing for Teens
Start Low: 0.5-1 mg (Yes, this is much lower than the 5-10mg bottles at the store) Timing: 90 minutes before target sleep time Max Dose: 3-5 mg (higher doses can cause grogginess, nightmares) Important: Melatonin is NOT a sedative. It signals “time for bed,” but doesn’t knock you out.
DO NOT: Use melatonin gummies (inconsistent dosing, too much sugar) DO: Use liquid or sublingual tablets for precise dosing
What If Dark Therapy Isn’t Enough?
If after 2 weeks of strict dark therapy, teen is still:
- Not falling asleep before midnight
- Waking up multiple times
- Getting <6 hours total sleep
Next Steps: 1. Medication Adjustment: Talk to psychiatrist about: - Trazodone (50-100mg) - sedating antidepressant - Seroquel (25-50mg) - atypical antipsychotic, very sedating - Clonidine (0.1mg) - blood pressure med, sedating side effect 2. Sleep Study: Rule out sleep apnea (common in teens with bipolar)
Troubleshooting Common Sleep Problems
“My teen says they’re not tired”
Response: “Your brain isn’t making melatonin yet. That’s the ADHD. We’re using dark therapy to fix that. Put the glasses on anyway.”
“They sneak their phone at night”
Solution: - Charge phone in parent bedroom (non-negotiable) - Use parental controls to disable all apps except phone/text after 10 PM - If still an issue: Flip phone for sleep hours (yes, seriously)
“They fall asleep at 10 PM but wake up at 2 AM”
Possible Causes: - Medication wearing off: Talk to psychiatrist about extended-release versions - Anxiety: Waking with racing thoughts? May need evening dose of anti-anxiety med - Sleep apnea: Snoring? Gasping? Needs sleep study
“Weekend sleep schedule destroys our progress”
The Problem: “Social Jet Lag” - sleeping till noon on Saturday undoes weekday progress The Rule: Weekends can shift 1 hour MAXIMUM (If weekday bedtime is 10 PM, weekend is 11 PM max) Enforcement: Parents wake teen by 9 AM even on weekends (yes, they will hate you)
Alex’s Sleep Victory
After 4 weeks of dark therapy:
- Alex now falls asleep by 10:30 PM (was 2 AM)
- Getting 7-8 hours of sleep (was 4-5)
- Mood stabilized (no hypomanic episodes)
- Grades improved (can focus in class)
Sarah says: “I didn’t believe it would work. It seemed too simple. But it was the single most effective intervention we did.”
The Takeaway
Sleep is not optional. It is medication. It is mood regulation. It is crisis prevention.
For teens with Bipolar + AuDHD:
- 7-9 hours of sleep = baseline stability
- <6 hours for 3+ days = mania risk
- Dark Therapy = most effective non-medication intervention
The Dark Therapy Schedule (Summary): 1. 7 PM: Blue light glasses on, dim lights 2. 9 PM: Melatonin dose (0.5-3mg) 3. 10 PM: Lights out, phone out of room 4. Consistency: Every single night, including weekends
It’s not glamorous. It’s not high-tech. But it works.