Managing the Rage
The Explosion
Whether it’s an Autistic Meltdown or a Manic Rage, the result is the same: The “Red Zone.” Logic does not work in the Red Zone. Consequences do not work in the Red Zone. Only Safety and De-escalation work.
Case Study: The Broken Window
Leo Rivera (16) is in the kitchen. He is pacing. His breathing is shallow. “I need the car keys,” he says. His voice is tight. “You can’t drive right now, Leo,” his dad, Mateo, says calmly. “You haven’t slept.” “GIVE ME THE KEYS!” Leo screams. He picks up a heavy ceramic bowl and hurls it through the kitchen window. Glass shatters everywhere. Mateo’s instinct is to scream back. “LOOK WHAT YOU DID!” But Mateo knows the rule. He takes a breath. He drops his shoulders. He becomes a statue. “I see you are angry,” Mateo says, his voice flat and boring. “I cannot give you the keys. But I can make you a sandwich, or I can leave the room.” Leo screams again, but he doesn’t throw another bowl. The “fuel” (Mateo’s reaction) has been cut off.
Understanding the Escalation Ladder
Both Autistic Meltdowns and Bipolar Rages follow predictable escalation patterns. Knowing where your child is on the ladder helps you choose the right intervention.
Meltdown Escalation Stages (Autistic/AuDHD)
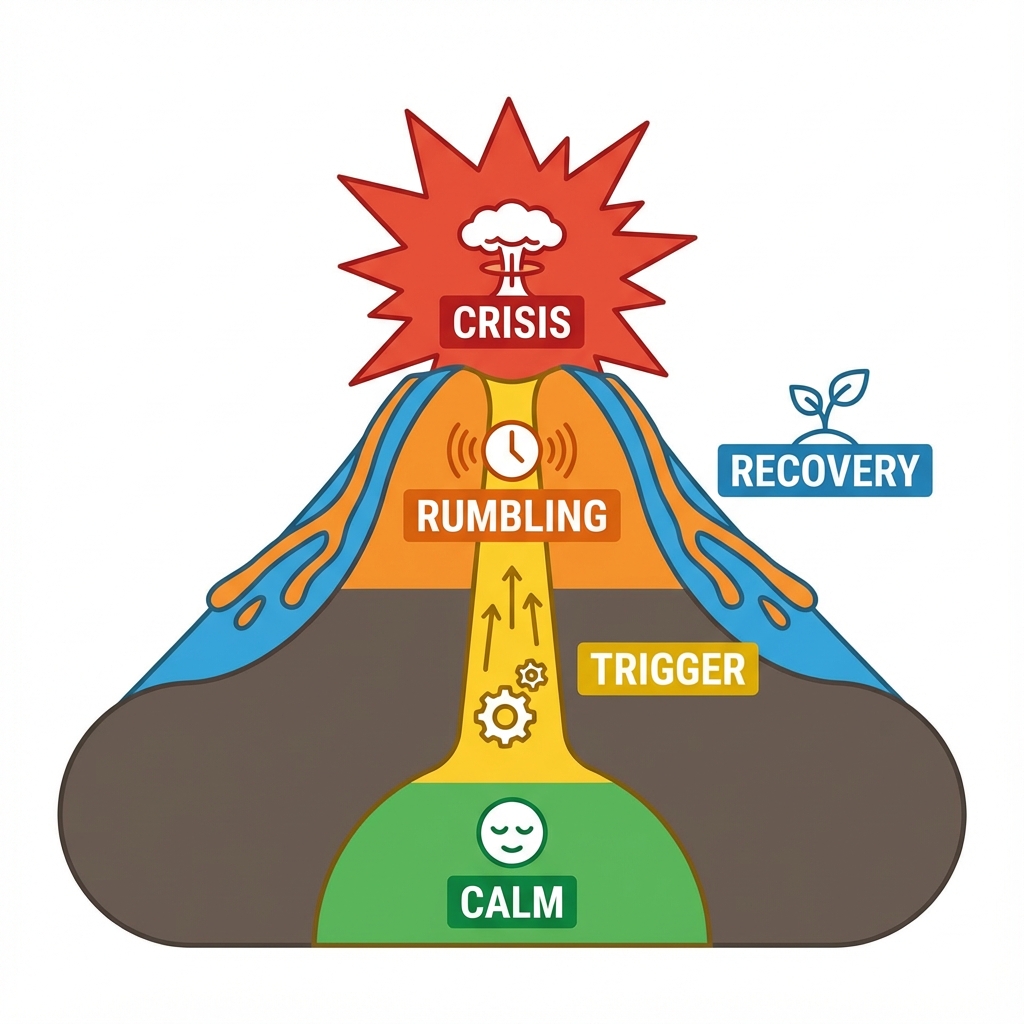
- Stage 1 (Calm): Regulated, responsive. Intervention: Build coping skills.
- Stage 2 (Trigger): Sensory overload, routine change. Intervention: Remove trigger, offer sensory tools.
- Stage 3 (Rumbling): Fidgeting, pacing, quiet. Intervention: Reduce demands, offer choices.
- Stage 4 (Escalation): Louder, more agitated. Intervention: Low stimulation, calm voice.
- Stage 5 (Crisis): Screaming, hitting, fleeing. Intervention: Safety only. No talking.
- Stage 6 (De-escalation): Energy fading. Intervention: Gentle reassurance, space.
- Stage 7 (Recovery): Exhausted, shame. Intervention: Rest, no debriefing yet.
Mania Escalation Stages (Bipolar)
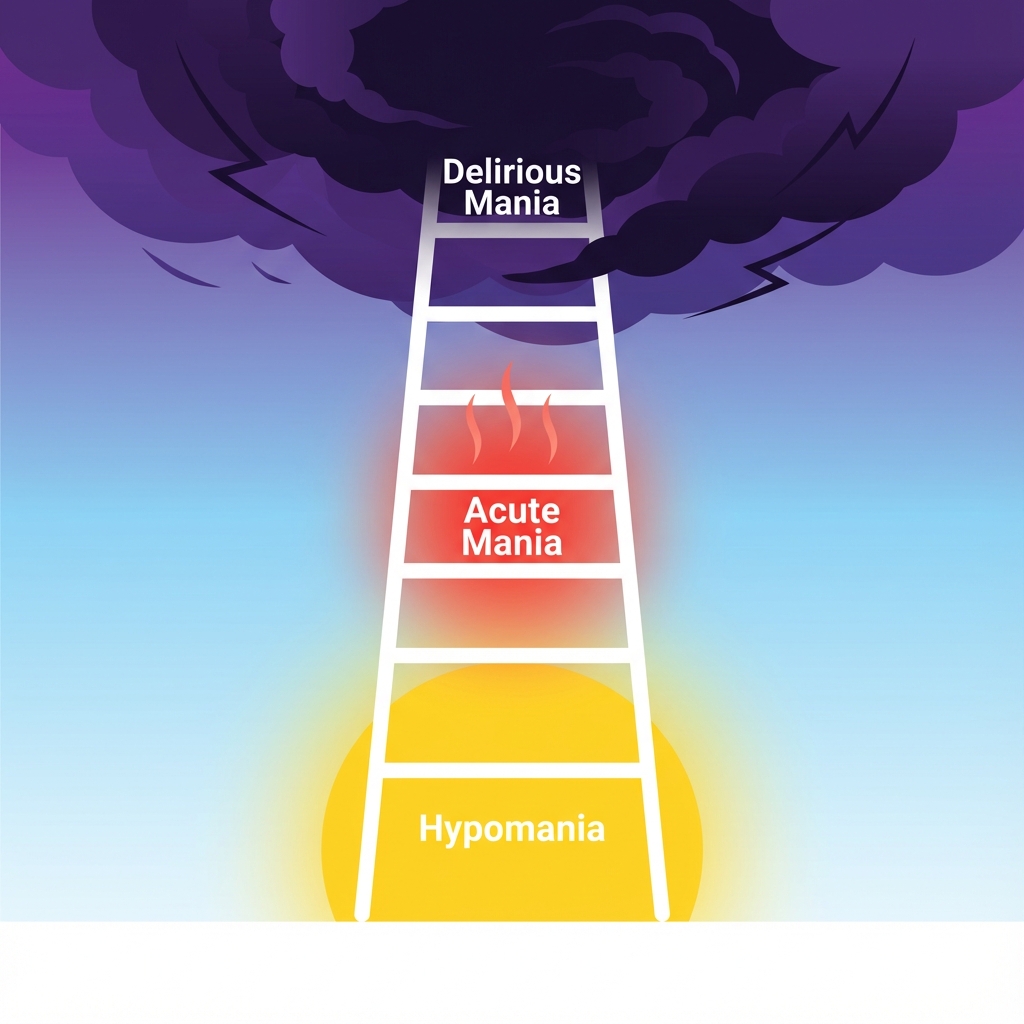
- Hypomania: Decreased sleep, racing thoughts, impulsive. Intervention: Increase medication, enforce sleep routine.
- Acute Mania: Rage, grandiosity, no sleep. Intervention: ER or crisis team.
- Delirious Mania: Psychosis, confusion, aggression. Intervention: HOSPITALIZE.
De-escalation 101
- The “Boring Face”: Do not mirror their emotion. If they are screaming, you must be a statue. Neutral face, low voice.
- Low Stimulation: Turn off the TV. Dim the lights. Get siblings out of the room. Reduce the sensory load immediately.
- Strategic Disengagement: “I love you too much to argue with you when you are hurting. We will talk about this later.” Then walk away (if safe).
Low Stimulation Zones
Every home needs a “Crash Pad.” - Not a Punishment: It’s not a “Time Out” corner. It’s a “Recovery Zone.” - The Setup: Bean bag, weighted blanket, noise-canceling headphones, dimmable lamp. - The Script: “I can see your engine is running hot. Let’s go to the Crash Pad to cool down.”
Protocol: The Hospital Decision Tree
When do you go to the ER?

What “Call 911” Means
- Request a CIT (Crisis Intervention Team) Officer: These officers are trained in mental health crises.
- Say: “My child is in a psychiatric emergency. They are Bipolar and autistic. I need a CIT officer.”
- Do NOT Say: “My child is being violent.” (This invites a use-of-force response.)
What Hospitalization Achieves
- Safety: Prevents suicide or serious harm.
- Stabilization: Aggressive medication management (IV meds, daily monitoring).
- Respite: Gives the family a break to recover.
What Hospitalization Does NOT Achieve
- “Fixing” the child: It stops the crisis, but it doesn’t cure Bipolar.
- Long-term care: Most stays are 5-7 days. Then you’re back home.
Protocol: The De-escalation Script & Safety Plan
The Script (Tape this to your fridge): - Step 1: Validate (“I see you are angry.”) - Step 2: Set Boundary (“I cannot let you break the door.”) - Step 3: Offer Choice (“You can sit on the bean bag or go to your room.”)
The Safety Plan: - Weapons: Remove all knives/sharps from the kitchen if mania is escalating. - Siblings: Have a code word (e.g., “Pineapple”) that tells siblings to go to their rooms and lock the door immediately. - 911: Know your threshold. If you are afraid for your life, make the call. Ask for a CIT (Crisis Intervention Team) officer. - Post-Crisis Review: After the crisis, document what happened. What were the triggers? What worked? What didn’t? Use this data for the next appointment.